What
is Neisseria gonorrhoeae and which
antimicrobial
therapies have been used?
| What
is Neisseria gonorrhoeae?
The prevalence
of gonorrhea (Neisseria gonorrheae)
in the United States and abroad, especially under-developed and developing
countries, has decreased in the last two decades. As of recently,
though, higher rates of infection have been reported due to the increase
of antimicrobial -resistant gonococci (Knapp
et
al., 1994). Gonorrhea is a very common infectious bacterium, a
Gram negative, fastidious,
diplococci, that can grow and rapidly multiply in the mucous membranes,
especially the mouth, throat, and anus of males and females, and the cervix,
fallopian tubes, and uterus of the female reproductive tract. Uncomplicated
gonorrhea affects approximately 650,000 persons per year (WebMD,
1999). This bacteria can be passed through sexual contact (vaginal,
oral, or anal), even without ejaculation, or spread from the mother to
child at birth. However, the spread and transmission of gonorrhea,
along with other sexually transmitted diseases, can be prevented using
condoms and other safe sexual practices.
|
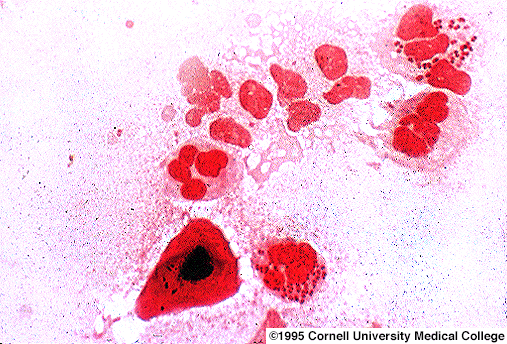
Intracellular
Gram negative diplococci
|
Symptoms
In females, mild
symptoms are usually present that resemble a bladder or vaginal infection;
or sometimes they are not even present, making it difficult to treat in
an efficient fashion. Symptoms can appear within 2-5 days for males,
but may not be present in females for over 30 days. The following
include painful urination and bloody or yellow vaginal or penile discharge,
which if left untreated can develop into pelvic inflamatory disease (PID)
for females, and swollen and painful testicles in males (epididymitis)
(WebMD). The presence of gonorrhea
can be be diagnosed using a Gram stain test, which will turn red for Gram
negative bacteria.
Antibiotics
used to treat it
Gonnorrhea is easily
treated through antibiotics; however, the estimated cost of treating gonorrhea
in the United States is $56 million each year (CDC
Update, 2000). Small amounts of penicillin,
and later on tetracycline, was the standard
treatment for gonorrhea since the emergence of antibiotics in the 1940s.
During the Vietnam War, the use of penicillin and tetracycline used to
treat
uncomplicated gonorrhea became more and more resistant as new strains mutated
(WebMD, 1999).
In 1963, the first
quinolone antibiotic, nalidixic acid, was approved by the Food and Drug
Administration for the treatment of urinary tract infections; however,
it had several limitations, such as it had a narrow spectrum of activity,
and bacteria quickly developed resistance to it (CTR,
1997). Modifications to nalidixic acid were made based on structure
activity relationships in the 1980s and these revisions, through adding
a fluorine to the 6 carbon, were responsible for improving activity of
this newly formed fluoroquinolone to include Gram positive organisms and
more Gram negative speices, such as Pseudomonas
aeruginosa and Neisseria gonorrhoeae (CTR,
1997). These have become an increasingly important addition to
antibiotic resources, unfortunately, the United States has now declared
this development and spread of bacterial resistance a major public health
threat.
The Centers for
Disease Control and Prevention (CDC) currently recommend an antibiotic
regime of 500mg single-dose ciprofloxacin and
400mg ofloxacin as broad-spectrum fluoroquinolones
and cephalosporins, respectively, to treat
uncomplicated gonorrhea (CDC, 2000).
Unfortunately, prior to 2000, N. gonorrhoeae's resistance
to ciprofloxacin was documented in Canada, Australia, United Kingdom, Hong
Kong, and the United States; fluoroquinolone resistance has also been reported
in the United States, but isolate frequently in the Far East (CDC,
2000). In order to monitor and track the susceptibility of N.
gonorrhoeae strains, the CDC has instituted the Gonococcal Isolate
Surveillance Project (GISP), which is a cooperative group of twenty-six
sexually transmitted disease clinics across the United States that collect
gonorrhea specimens and send them to regional offices for resistance diagnosis
(CDC Update, 2000). This program has
detected resistance cases in Hawaii and Missouri; for example, in 1999,
a group of twelve patients in Kansas City, MO became infected with gonorrhea
that had increased resistance to azithromycin.
Home
Next
